Millions of Americans experience acid reflux every day. Most don’t know if it’s severe enough and lasts long enough, in the worst cases acid reflux can increase the risk of esophageal cancer.
When that happens, the symptoms usually become apparent as a slow but distinctive change in one’s usual reflux symptoms, or new difficulties with eating or swallowing.

William Emert
William Emert is one such patient who had years of reflux and found out the hard way.
“I thought I was healthy,” Emert says. “I didn’t listen to my body.”
Since his cancer diagnosis in May 2021, cutting-edge treatment including robotic-assisted surgery at Fort Sanders Regional Medical Center took Emert from a life-threatening illness to the restored quality of life he enjoys today.
Prolonged gastroesophageal reflux disease (GERD) can damage the lining of the esophagus, making it easier for abnormal cells to take over and possibly transform into a type of tissue called Barrett’s esophagus, a condition which raises the risk of esophageal cancer.
“I was feeling run-down at work, just feeling bad, weak and tired all the time. I kept ignoring it and ignoring it,” Emert says.
Emert’s wife encouraged him to see a doctor and when he finally did, he was shocked by the news that came from his blood work.
“The doctor said ‘We’ve got to send you to the emergency room immediately. You’ve got internal bleeding, and I think you might have cancer,’” Emert recalls. “It blows you away.”
A very large tumor had engulfed the lower third of Emert’s esophagus, draping down onto his stomach. After the diagnosis of cancer was confirmed, he underwent preoperative chemotherapy and radiation to shrink the tumor. Surgery was planned to complete the treatment.

Michael Antiporda M.D.
Michael A. Antiporda MD is a fellowship-trained foregut surgeon (specializing in procedures for the esophagus, stomach and upper small intestine) at Fort Sanders Regional Medical Center. He recommended robotic-assisted laparoscopic surgery to remove the tumor and reconstruct Emert’s GI tract in the most minimally invasive way possible.
“This is major surgery in potentially treacherous territory involving the chest, abdomen and neck,” Dr. Antiporda says. “It’s a highly complex operation that’s not done in high volume in many places, but at Fort Sanders Regional we’re able to do many complicated cancer surgeries like these with good outcomes.”
The Right Hospital
Fort Sanders Regional was the first hospital in East Tennessee with robotic-assisted surgery. The medical center has continually updated and added to its robotic program since then. This technology allows surgeons to offer the most advanced and minimally invasive procedures for a wide array of indications.
“Mr. Emert underwent robotic transhiatal esophagectomy, which I performed using multiple very small abdominal incisions and one small left-neck incision. The robot is clutch for doing an operation like this because it permits a surgeon to use tiny incisions to operate comfortably and safely in what would otherwise be a very tight and limited space,” Dr. Antiporda says.
“The alternative to this type of surgery would have been to make large painful incisions in the upper abdomen or between the ribs, which take significantly longer to recover from.”
The tumor was removed in August 2021. Although it was major surgery, Emert was able to go home in less than a week, fully realizing the advantage of faster recovery that is often seen with robotic surgery. He was pronounced “cancer-free” on Aug. 14.
Lessons to Learn
Today Emert has a smaller stomach space that limits the amount of food he can eat in one sitting, but there are no restrictions on his diet. His quality of life has returned, and he and his wife go on adventures from fishing to foraging mushrooms.
“I feel great. I had forgotten what it was to be healthy because I just got so used to feeling bad,” he says.

William Emert
Through it all, Emert has learned some important life lessons. Among them are the importance of taking time to enjoy and appreciate life, along with the importance of self-awareness when it comes to good health.
“Listen to your body, because your body knows when something’s wrong. I learned the hard way,” Emert says. “I’m just glad to be here, and it wouldn’t have been possible without the doctors that I had. I don’t think I’ve met a better doctor – or person – in my whole life than Dr. Antiporda.”
Dr. Antiporda says uncontrolled GERD is the most common underlying cause of esophageal type of cancer and it’s important to see a doctor for ongoing reflux that causes pain or trouble swallowing. In the event that a cancer diagnosis does come as a result of GERD, Fort Sanders Regional Medical Center is ready with the knowledge, experience and tools for the best possible outcome.
To learn more about surgery at Fort Sanders Regional visit FSRegional.com/Surgery or call 865-673-FORT (3618).
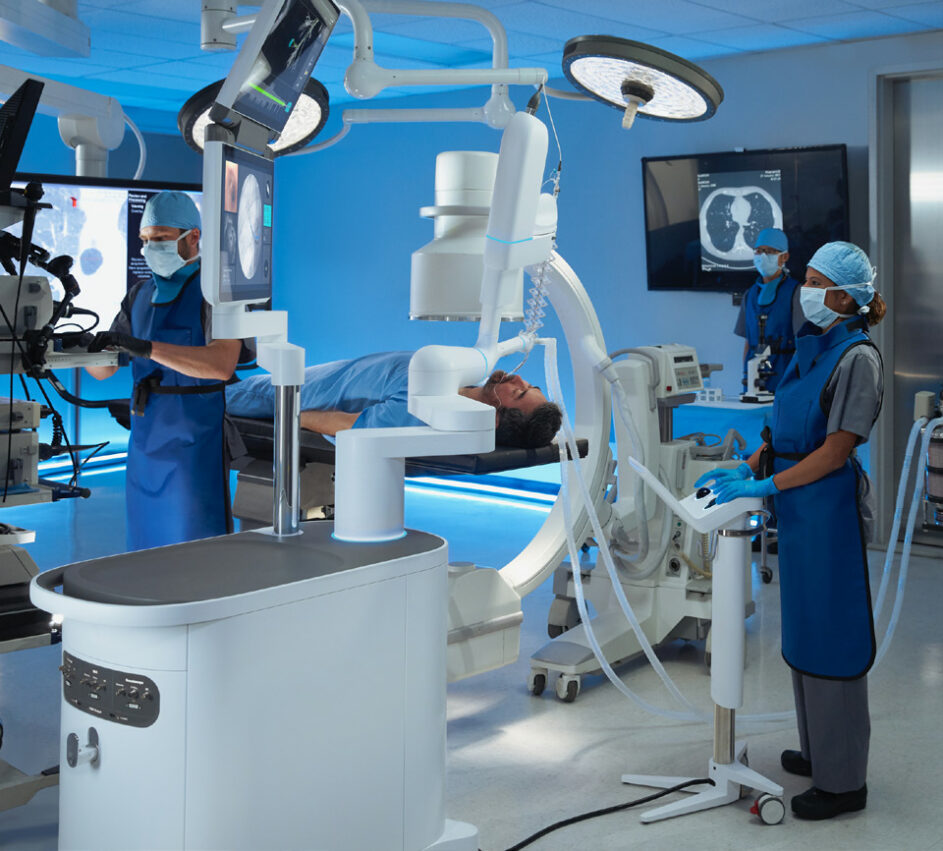
Robotic-Assisted Lung Biopsies at Fort Sanders Regional
Fort Sanders Regional Medical Center has announced the addition of a robotic-assisted bronchoscopy platform for minimally invasive lung biopsies. This technology is first of its kind in East Tennessee and will allow specially trained Fort Sanders Regional physicians to obtain tissue samples in deep regions of the lung, where many early-stage tumors are found.
The shape-sensing robotic-assisted bronchoscopy features an ultra-thin, ultra-maneuverable catheter that allows navigation by the physician far into the peripheral lung. It provides additional stability and precision needed for biopsy compared to manual techniques.
As with other robotic-assisted surgery platforms, the physician is in complete control of the robot and navigates to the target along a planned path. The catheter can move 180 degrees in any direction to pass through small, difficult-to-navigate airways and around tight bends. The robot’s peripheral vision probe provides direct vision during navigation.
Once the pulmonary nodule is reached, the catheter locks in place and a flexible biopsy needle passes through the catheter. After advancing around the bends of the catheter, the needle deploys into the target location on a straight path.
“This technology revolutionizes how we approach lung nodules – it’s like GPS for the lungs. It will allow us to reach peripheral areas of the lungs that were difficult or impossible to reach before,” Varun Shah MD, interventional pulmonologist, said. “Ultimately, we’ll be able to diagnose lung cancer earlier and start treatment earlier, providing more opportunity for a successful outcome.”
“Lung nodules are often found in difficult-to-access locations,” David B. Graham, MD, FACS, a thoracic surgeon at Fort Sanders Regional, said. “This new equipment allows our specialized pulmonologists to obtain an earlier, more accurate diagnosis. Finding lung cancer earlier allows for earlier treatment and, therefore, better patient outcomes. I’m excited about the benefits for our lung nodule patients here in Knoxville.”
The hospital performed its first lung biopsies with the endoluminal system in mid-February.
Information provided by Covenant Health.